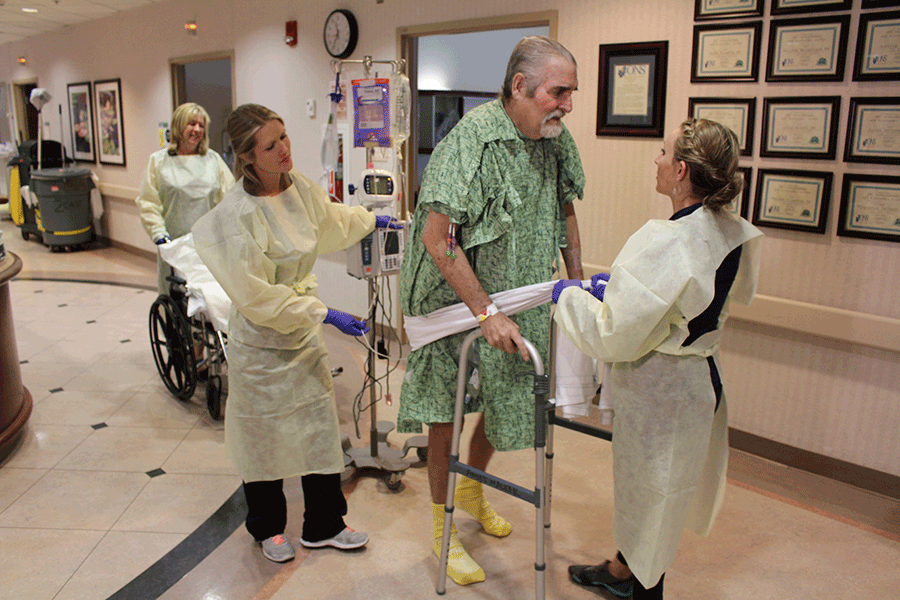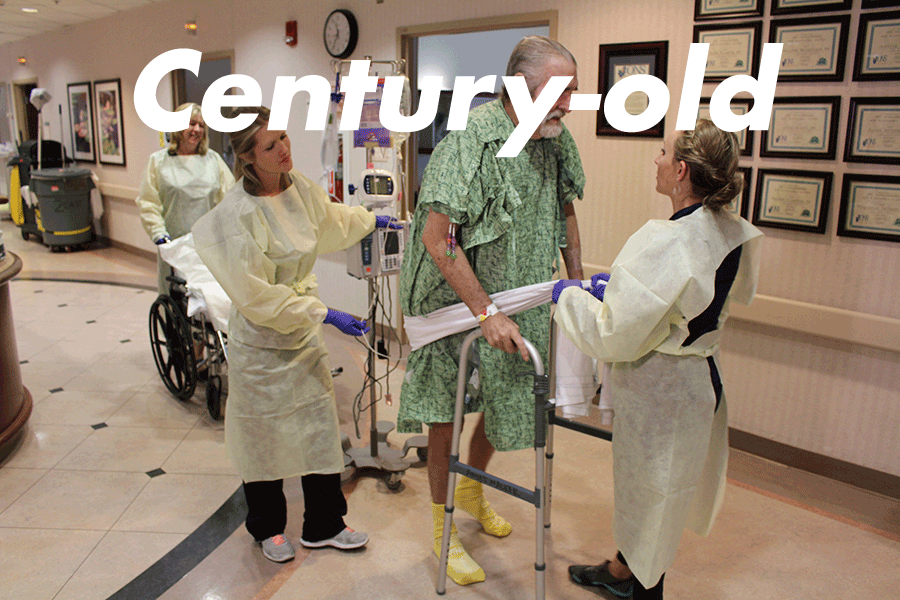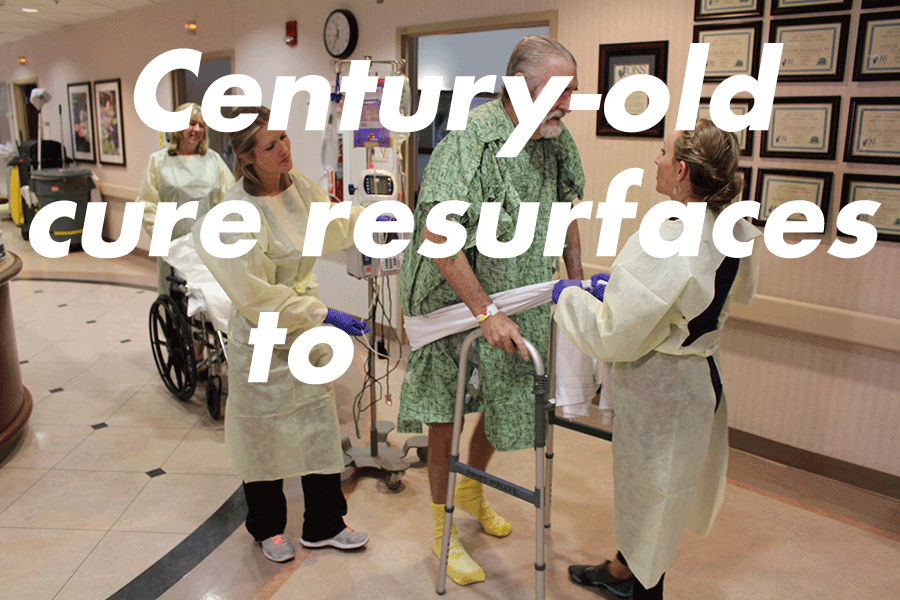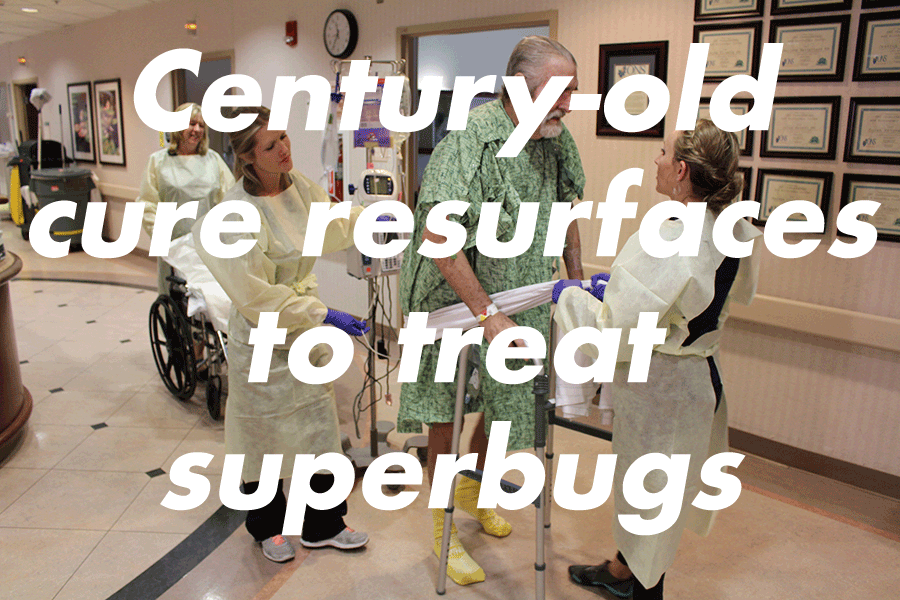-
Credits
- Stories by:
- Laura Kane & Aleksandra Sagan
- Edited by:
- Sunny Freeman & Kevin Ward
- Layout & Graphics by:
- Lucas Timmons
- Graphics by:
- Sean Vokey
- Produced by:
- Megan Leach

Canadian Press reporters travelled to South Africa and India to investigate the growing epidemic of drug resistance, which experts describe as the single greatest threat to human health on the planet.
This is the first story of a six-part series exploring how the unfettered use of antibiotics pushes humanity closer to a post-antibiotic era in which common infections may be impossible to treat.
The R. James Travers Foreign Corresponding Fellowship partly funded this series. It commemorates Jim Travers's career and aims to enable significant foreign reporting projects by Canadian journalists to give Canadians first-hand, in-depth coverage of stories beyond the country's borders. Travers spent six years reporting from Africa and the Middle East and deeply believed in the power of international reporting.
Antimicrobial resistance, or the growth of micro-organisms that fight off the drugs used to treat them, has been rising in Canada and globally for decades. The unfettered use of antibiotics in humans and animals, coupled with environmental contamination, has helped create superbugs and made common diseases more difficult to cure. An estimated 700,000 people worldwide die annually from drug-resistant strains of bacterial infections, HIV/AIDS, tuberculosis and malaria. Unless urgent action is taken, experts warn that by 2050, the annual death toll will soar to 10 million worldwide — dwarfing cancer — and drug resistance could cost the global economy US$100 trillion overall. Developing countries will experience the worst impacts, but countries like Canada are not immune: widespread international travel and trade help bacteria spread across borders.
A 2013 study estimated 60,000 infants in India die annually from sepsis caused by antimicrobial-resistant infections, and the expert who calculated the figure now believes the rate to be double that. Doctors increasingly treating babies with colistin see even those just born carry a frightening resistance to the drug. They worry about what to do when that last line of defence fails. The situation is desperate and not confined to developing countries. In Canada, hospitals also grapple with the rise of dangerous superbugs. The rapid spread of a highly resistant enzyme from South Asia to the West illustrates the global nature of drug resistance.
In India and Canada, farmers give their animals antibiotics to fatten them up, prevent disease or treat sickness. Many farmers say antibiotics are critical to ensure the health and safety of their livelihood, but the practice also carries a dangerous cost for humans. Farmed animals use a staggering amount of antibiotics; in some countries, they consume more than people. Such unfettered use helps to create and spread superbugs, bacteria resistant to antibiotics responsible for killing an estimated 1.5 million people each year. The antibiotics animals consume can eradicate some bacteria, but allow strains that are drug-resistant to thrive and transfer to humans through meat or the environment, making people sick with sometimes fatal drug-resistant infections.

Hyderabad, the self-proclaimed "bulk drug capital of India," churns out a steady stream of generic drugs, including antimicrobials, for global consumption. Dozens of facilities hold licences to export to Canada. The worldwide overuse of antimicrobials in humans and animals is accelerating dangerous drug resistance, killing an estimated 1.5 million people a year and pushing medical care closer to a post-antibiotic era in which common diseases are no longer curable. But resistance also appears to be growing in the environment. Some researchers say rivers, lakes and groundwater in Hyderabad contain elevated levels of antibiotics and drug-resistant superbugs. Pharmaceutical waste and substandard sanitation are breeding antimicrobial immunity, say experts, who contend the West's support of cheaply produced drugs makes it complicit.

Drug-resistant TB wreaks havoc on the body. Infected people cough so violently they spit up blood and pieces of their lung lining. Their chest aches and fever spikes. Their body weight plummets and they transform into a skeletal frame. Drug-resistant tuberculosis is the world's deadliest superbug. It develops when bacteria that causes tuberculosis, a disease believed to be as old as mankind, stops responding to drugs used to treat it, largely because health-care workers improperly prescribe medicine or patients stop treatment early. Infected people can spread it through the air when they cough. Often, a victim's only fault is breathing.
Western doctors mostly shelved phage therapy as a treatment after the advent of antibiotics. But the drugs, once considered a medical marvel, no longer work against a growing number of bacterial infections. Rampant misuse and overuse helped spur the growth of antibiotic-resistant bacteria, resulting in superbugs that now kill an estimated 1.5 million people each year. While superbugs proliferate, antibiotic discovery has stalled. For pharmaceutical companies, there is little profit incentive to invest in drugs that quickly cure patients; medicine for chronic conditions presents a more tempting return on investment. That leaves patients whose infections don't respond to antibiotics and whose doctors run out of new medicines to prescribe, turning to the century-old practice.